Featured
Tags
Share
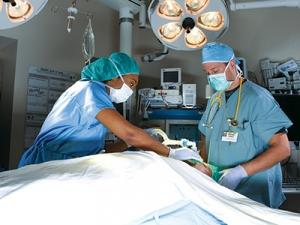
Love anatomy and physiology? The chance to do innovative things in a highly disciplined environment? Surgical nursing might be the specialty for you.
Lori Armbruster, MSN, RN, is Faculty Chair at Chamberlain’s St. Louis campus and a surgical nurse with 28 years of experience in the OR. She explained that surgical, or perioperative, nursing may have a long learning curve, but for nurses who love technology and organization, it can make for a very satisfying career.
Here are five things to know about this specialty:
1. Scrub or circulate?
Surgical nurses care for patients before, during and after surgery. Some nurses will prepare the patient for surgery, others serve during the actual procedure and additional nurses work in the recovery area.
During the surgery itself, there are two main roles for nurses: scrub nurse and circulating nurse. There may be just one nurse in each of these roles, or there may be multiple, depending on the complexity of the case.
Scrub nurses literally scrub their hands and arms with surgical soap and don a surgical gown and gloves. They anticipate the surgeon’s needs, selecting and passing instruments and supplies.
The circulating nurse acts a runner and helps out wherever needed.
“This is the person who walks around the perimeter of the room and is the monitor of everything going on,” said Professor Armbruster. “They’re the helper for anesthesia, the help for the scrub person. They answer phones and beepers and bring you supplies. If you drop something, they pick it up and re-sterilize it and bring it back.”
2. Organization is a must.
Surgical nurses are part of a well-orchestrated team that also includes staff doctors, anesthesiologists or nurse anesthetists, surgeons, surgery techs and maybe even residents or medical students.
Everyone has a job, and everything has a place. That makes surgical nursing a great fit for nurses who love order and organization.
“Surgery is a very controlled, disciplined environment,” said Professor Armbruster.
Complications do arise, but even during those moments, the sense of planning and protocol is palpable.
“It’s not like the chaos of the ED, where you’re rushing down the hallway with someone who’s not breathing,” said Prof. Armbruster. “In the OR, you can say, ‘I gave this drug and I know that in 10 seconds, I’m going to be intubating this patient.’ That’s the difference.”
3. Teamwork is crucial.
One of the most important prerequisites for a surgical nurse is the ability to work in a team setting.
For example, if you’re scrubbed in, you can’t go get your supplies out of the other room – you have to depend on the circulating nurse.
“Your team has your back and you have their back,” said Prof. Armbruster. “You work with a team of people so closely that after a while, you can almost just look at their face and know something’s wrong or they need something and you don’t need to say a word. That develops when you’re working in a very specialized team and everyone’s on the same page.”
4. There’s a lot to learn – but also a lot of places you can go.
While nursing school provides a solid foundation, the bulk of what you need to know about tools and techniques comes from one-on-one training with a preceptor.
“You have to put a lot of time in it, to learn all the different instruments and procedures,” she explained. “I can tell you it’s probably two years before you feel really comfortable in the OR.”
Once you’re trained, however, you’ve got lots of options.
“There’s a ton of stuff you can do with it – outpatient surgery center, OR, be on call on the weekends.”
Perioperative nurses can also choose to specialize even further, into orthopedic, cardiovascular, neuro or other surgical subspecialties.
“You can get really good at one service and when they get call-ins, you’ll get called in with that same set of doctors and nurses,” said Prof. Armbruster. “It’s like a team, like a family.”
5. It’s not the easiest specialty to break into, but it’s not impossible
It’s not very common for a new graduate to be hired for a perioperative nursing position, explained Professor Armbruster. A more likely scenario is for a new nurse to gain a few years of experience and then transition into the specialty.
For example, Prof. Armbruster began as a floor nurse in pediatrics. She was eventually assigned to the recovery room three days a week.
“It was a very small hospital, and you could watch through the windows in recovery and watch surgeries going on – that’s how close we were,” she said. “I was always watching surgery and thinking, ‘If they need help, come and get me. I want to help.’”
Eventually, a position opened in the OR, and the rest is history.
For nurses who are interested in making a similar transition into the OR, Prof. Armbruster suggests you take a few steps.
First, she said, “Express the interest. If you say it enough times, people might hear you and there might be a possibility out there.”
Next, prove to others that you’ve got the right stuff – meaning a collaborative personality and can-do attitude.
“Do everything and anything they ask you to do in your current job,” she advised. “If they tell you to assist in this or that, go do it. Never say ‘no’ to anything. The more willing you are to do things, the more they’ll see that you’re willing and able to be trained in a whole other nursing area.”
For more information on surgical nursing, visit the Association of periOperative Registered Nurses website – aorn.org.
By Danielle Logacho
More from Careers
Request More Information
To receive the Chamberlain University Program Guide, including associated career paths, please select a program of study.






